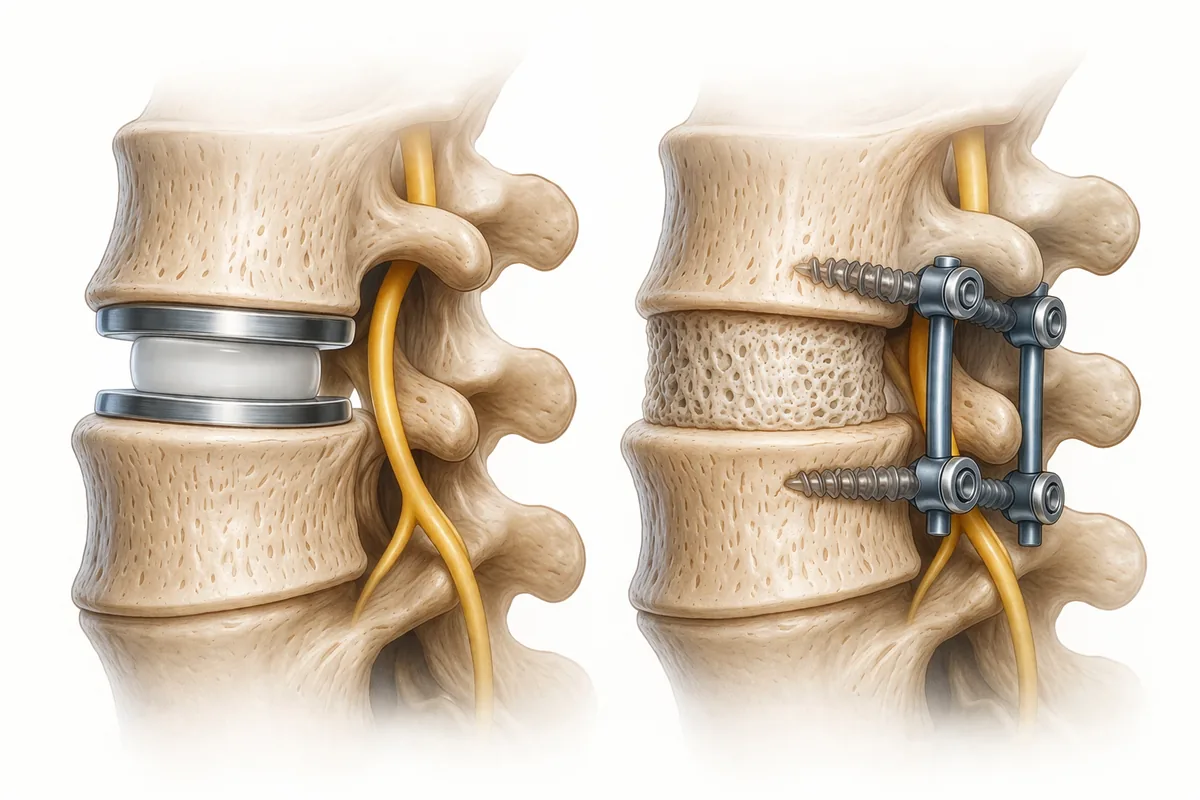
Understanding the Disc Replacement vs. Fusion Decision
When patients come to my office with a degenerated disc causing pain, numbness, or weakness, one of the first questions they ask is: "Why not just replace the disc instead of fusing it?"
It's a fair question. The theory behind artificial disc replacement is appealing—preserve motion in the spine, reduce stress on adjacent levels, and return patients to normal activity faster. But as a surgeon who trained at Mayo Clinic and has spent years studying spine outcomes, I've learned that theory doesn't always match reality.
This page explains what disc replacement is, what the research actually shows, and why I choose fusion for nearly all my patients.
What the Research Shows
The evidence on artificial disc replacement is clear, and it doesn't support the procedure's theoretical advantages.
Multiple peer-reviewed studies have shown no substantial advantage of disc replacement over fusion in terms of pain relief or functional outcomes. Patients undergoing fusion report pain reduction comparable to—or better than—those receiving artificial discs. When it comes to adjacent-level disease (degeneration at spinal levels above or below the surgical site), fusion and disc replacement perform similarly. Neither procedure prevents future degeneration better than the other.
What does differ is long-term failure rates. Artificial discs carry specific risks: implant wear, loosening, displacement, fracture, and infection. When these complications occur—and they do—patients often require revision surgery, which is more complex and carries higher morbidity than the original fusion would have.
The faster recovery time after disc replacement is real, but it's measured in weeks, not months. By one year post-op, fusion patients who undergo minimally invasive techniques achieve recovery times nearly identical to disc replacement patients. The early advantage disappears.
Why I Choose Fusion for My Patients
My practice philosophy is straightforward: recommend the procedure with the best long-term outcomes and lowest complication rates. For most patients, that's fusion.
Proven long-term durability. Fusion has been the gold standard for spinal reconstruction for decades. We have 20+ years of outcome data showing that fused segments remain stable, provide sustained pain relief, and allow patients to return to meaningful activity.
Superior pain control. Fusion addresses the underlying problem—instability and neural compression—by definitively stabilizing the spine. Patients report sustained improvement in pain and function. With disc replacement, you're asking the artificial device to perform a job the biological disc no longer can, and that job often exceeds the device's capability.
Lower revision rates. Fusion is durable. Yes, adjacent-level disease can occur at segments above or below a fusion, but that's true regardless of the index procedure. The difference is that fusion rarely fails at the fused level. Artificial discs, conversely, require revision surgery at a measurable rate, converting one surgical risk into two.
Motion preservation is oversold. Surgeons and device manufacturers often market disc replacement as "motion-preserving" compared to fusion. But here's the reality: a patient with severe degenerative disc disease already has compromised motion at that level. The disc is damaged. The anatomy is compromised. Inserting a device to restore motion to a pathological segment is theoretically appealing but clinically underwhelming. Patients who undergo fusion at one level show minimal functional limitation—they adapt, other segments compensate, and they move freely.
When Patients Ask About Disc Replacement
I'm transparent with every patient: I don't perform artificial disc replacement surgery. Not because I'm not trained in the technique, but because I don't believe it serves my patients' best interests.
Some patients have received a second opinion recommending disc replacement, and I always respect that. I explain my reasoning clearly: the research doesn't support superior outcomes, failure rates are concerning, and fusion offers durable, predictable results. I show them the literature. I answer their questions.
In nearly every case, patients choose fusion once they understand the evidence.
Patients occasionally ask if they should travel elsewhere for disc replacement. My honest answer: if you're a perfect candidate (single-level disease, young, no comorbidities, excellent bone quality), you might have acceptable outcomes with an experienced artificial disc surgeon. But "acceptable" isn't the same as "optimal." I recommend what I believe is optimal.
The Fusion Procedures I Recommend
For most patients with degenerative disc disease or herniation requiring decompression and stabilization, I offer several fusion approaches:
Anterior Cervical Discectomy and Fusion (ACDF) is ideal for cervical conditions. The procedure removes the damaged disc, decompresses the nerve root or spinal cord, and fuses the vertebrae using bone graft and instrumentation. Minimally invasive techniques reduce soft-tissue trauma and accelerate recovery.
Lumbar Fusion techniques include ALIF (anterior lumbar interbody fusion), PLIF (posterior lumbar interbody fusion), and TLIF (transforaminal lumbar interbody fusion). I select the approach based on your anatomy, the number of levels requiring fusion, and the location of stenosis or instability.
Laminectomy with fusion addresses patients with stenosis combined with instability. Removing the lamina decompresses the spinal cord while fusion prevents abnormal motion.
Minimally invasive techniques reduce muscle damage, bleeding, and post-operative pain while providing the same durable outcomes as open surgery.
All of these approaches leverage modern instrumentation, biologics, and surgical precision to achieve fusion rates exceeding 95% with excellent pain relief and functional improvement.
The Bottom Line
Disc replacement has its place in spine surgery. For a very select group of patients—primarily those with single-level disease, ideal anatomy, and specific patient factors—an experienced artificial disc surgeon might recommend it. But for the vast majority of patients with symptomatic degenerative disc disease or herniation, fusion is the superior choice.
I've built my practice on transparency and evidence. When a patient asks why I choose fusion over disc replacement, I show them the research, explain the outcomes, and discuss the risks. Nearly every patient agrees that durable, proven outcomes matter more than theoretical motion preservation.
If you're considering spine surgery and want an honest, evidence-based discussion of your options, I'd welcome the opportunity to evaluate you. You can reach my office in San Antonio or Houston to schedule a consultation.
Related Procedures:
When This Procedure Is Recommended
- Cervical or lumbar disc herniation
- Degenerative disc disease with persistent pain
- Radiculopathy or myelopathy from disc degeneration
- Conditions requiring single or multi-level spinal decompression
Surgical Techniques
- Anterior Cervical Discectomy and Fusion (ACDF)
- Lumbar Fusion (ALIF, PLIF, TLIF)
- Posterior Cervical Foraminotomy
- Laminectomy with Fusion
- Minimally Invasive Fusion Techniques
Frequently Asked Questions
Why does Dr. Cyr prefer fusion over disc replacement?
Research shows no substantial advantage of disc replacement over fusion for pain relief or function. Fusion has proven long-term durability and lower revision rates. Disc replacement carries specific risks like implant wear, loosening, and displacement.
Does disc replacement really preserve more motion than fusion?
Disc replacement is marketed as motion-preserving, but a severely degenerated disc already has compromised motion. Studies show fusion patients have minimal functional limitations—other spine segments compensate well.
What does the research say about adjacent-level disease?
Multiple peer-reviewed studies show no substantial difference between disc replacement and fusion in terms of preventing degeneration at adjacent levels. Both procedures have similar long-term adjacent-segment disease rates.
Is recovery faster with disc replacement than fusion?
Disc replacement does offer faster early recovery—measured in weeks. However, by one year post-op, fusion patients using minimally invasive techniques achieve recovery times nearly identical to disc replacement patients.
What is the revision rate for artificial discs?
Artificial discs carry specific failure risks requiring revision surgery. Fusion, by contrast, rarely fails at the fused level and has proven long-term stability over 20+ years of outcome data.

