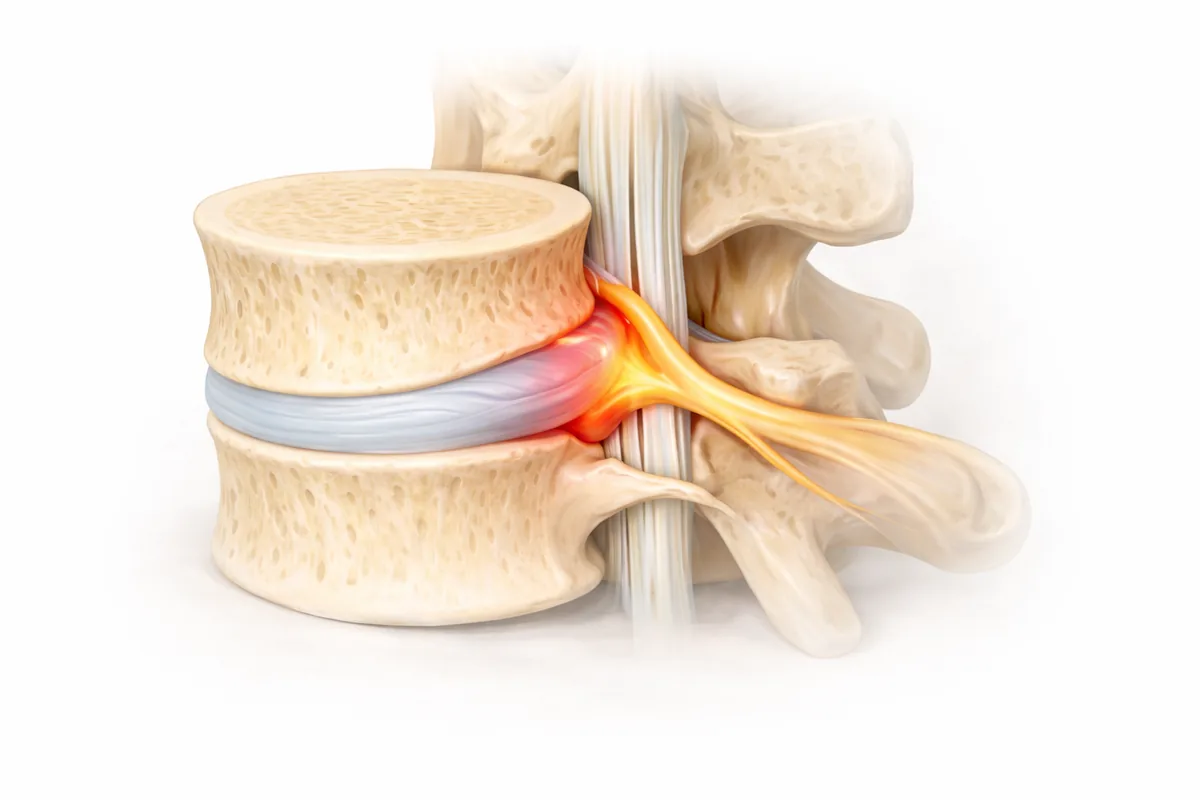
What Is a Pinched Nerve?
A pinched nerve—also called radiculopathy—occurs when a nerve root becomes compressed as it exits the spine. The nerve gets squeezed by bone, disc material, thickened ligaments, bone spurs, or swollen tissue, and that compression interrupts the nerve's ability to function normally. The result is pain, numbness, tingling, or weakness that radiates along the nerve's path into your arm or leg.
The key difference between a pinched nerve and just spinal pain is that the pain follows a nerve distribution. It's not just localized to your neck or back—it shoots down your arm or leg in a specific pattern. That characteristic radiating pain tells me exactly which nerve root is involved, which is crucial for diagnosis and treatment.
I see pinched nerves regularly in my San Antonio and Houston practices, and the good news is that most respond very well to conservative care. When surgery is needed, modern nerve decompression techniques offer excellent results.
What Causes Nerve Compression
Several spinal conditions can compress a nerve root as it exits the spine:
Herniated disc is a common culprit, especially in younger patients. When the disc's inner material protrudes backward, it can push directly on the nerve root emerging from that level, causing immediate inflammation and radiating pain.
Bone spurs (osteophytes) develop from osteoarthritis and degenerative changes over time. These bony growths encroach into the space where the nerve travels, narrowing the neural foramen—the small opening where the nerve exits the spine. This is particularly common in patients over 50.
Foraminal stenosis is narrowing of the neural foramen itself, preventing the nerve from passing through freely. This can result from a combination of disc bulging, bone spur formation, and facet joint arthritis.
Thickened ligaments, especially the ligamentum flavum at the back of the spinal canal, can compress the nerve root, particularly during extension of the spine.
Facet joint arthritis (facet hypertrophy) causes the small joints between vertebrae to enlarge, encroaching on the space where nerve roots travel.
Spondylolisthesis (vertebral slippage) misaligns the vertebrae, which stretches or compresses the nerve root as it exits.
Swelling from inflammation around the nerve can temporarily compress it, even without structural narrowing. This is why anti-inflammatory treatment is often effective early on.
Age, poor posture, heavy lifting with improper form, sedentary work habits, and prior spine injury all increase your risk. Repetitive strain and prolonged positions that compress the nerve—like hours of driving or desk work—can trigger or worsen symptoms.
How I Diagnose a Pinched Nerve
My diagnostic process identifies not just that you have a pinched nerve, but exactly where it's pinched and why. This precision guides every treatment decision.
Clinical examination comes first. I perform specific tests: nerve tension tests (like the straight leg raise for lumbar nerves or the upper limb tension test for cervical nerves), manual muscle testing of muscles controlled by each nerve root, reflex testing, and sensation mapping. The pattern of weakness, numbness, and reflex loss tells me precisely which nerve root—C5, C6, C7, L4, L5, or S1—is compressed.
Imaging with MRI is the gold standard for showing nerve compression. MRI gives me excellent detail of the disc, spinal canal, ligaments, and nerve roots, so I can visualize the exact site and cause of compression. I can see bone spurs, disc material, ligament thickening, and foraminal narrowing.
Sometimes nerve conduction studies or EMG (electromyography) are helpful to confirm that the nerve is truly compressed and to assess the degree of dysfunction. These tests measure electrical activity in the nerve and muscles.
Clinical correlation is essential. I've seen patients with MRI findings that don't match their symptoms. That's why the physical exam—correlating imaging with your specific pain pattern, weakness, and numbness—is what truly guides my recommendations.
Conservative Treatment: The Starting Point
Most pinched nerves respond well to non-surgical care, and that's always my first-line approach. Surgery is reserved for those who fail conservative therapy or have progressive neurological loss.
Physical therapy is foundational. A pinched nerve PT program emphasizes:
- Nerve mobility work: Specific stretches and movements help the nerve glide freely through areas of potential compression. For cervical nerves, this might include gentle neck flexion and rotation; for lumbar nerves, hip and spinal mobility.
- Core stabilization: Strong deep abdominal and spinal muscles reduce pressure on nerve roots by providing stability and proper alignment.
- Postural correction: Many patients have movement or posture habits that compress the nerve—tight hip flexors with lumbar compression, or forward head posture with cervical compression. Retraining these patterns is critical.
- Strength and endurance: Gradual strengthening of muscles controlled by the compressed nerve prevents atrophy and improves function.
Most patients experience significant improvement within 4-8 weeks of consistent PT, especially when symptoms are not severe.
Anti-inflammatory medications including NSAIDs and short-term muscle relaxers reduce swelling around the compressed nerve and can provide enough relief to allow better PT participation. I avoid long-term opioid use for radiculopathy—they mask the problem without addressing it.
Epidural steroid injections are highly effective for pinched nerves. The steroid is delivered directly into the epidural space around the compressed nerve root, reducing inflammation and providing relief that often lasts weeks or months. This window of reduced pain allows PT to be more effective. I typically recommend up to three injections spaced 2-3 weeks apart if the first provides benefit—after that, results usually diminish.
Activity modification is critical. I counsel patients to avoid positions or movements that reproduce their radiating pain while maintaining gentle mobility. For a pinched cervical nerve, this might mean avoiding prolonged neck rotation; for lumbar, avoiding forward bending or heavy lifting.
Time and natural resolution matter. Many herniations gradually reabsorb, inflammation naturally decreases with conservative care, and the nerve can recover function. Patience, consistency with PT, and activity modification are your allies.
When Surgery Becomes Necessary
I recommend surgical intervention for pinched nerves when:
- Conservative therapy fails after 8-12 weeks: You've completed PT, tried injections, modified activities, and you're still significantly limited and in pain
- Neurological deficit progresses: Your weakness is worsening despite non-surgical treatment, signaling risk of permanent nerve damage
- Severe pain impairs quality of life: Pain is so severe that you cannot work, participate in daily activities, or sleep adequately despite medical management
- Acute cauda equina syndrome: Bowel or bladder dysfunction or bilateral leg pain requires urgent decompression—this is a surgical emergency
Surgical Options: Decompression and Fusion
When surgery is indicated, I tailor my approach to the underlying pathology.
Laminectomy or foraminotomy is my most direct approach. I remove small portions of the lamina (back of the vertebra) and/or enlarge the neural foramen to decompress the nerve root at its exit point. This is particularly effective for foraminal stenosis or bone spur compression. For a single-level pinched nerve without instability, decompression alone often provides durable relief.
Laminectomy-fusion is my choice when there's underlying instability—a slipped vertebra, significant disc degeneration causing hypermobility, prior spine surgery at that level, or recurrent compression at the same site. Fusion stabilizes the segment after decompression, preventing future compression and providing superior long-term outcomes. I perform minimally invasive fusion using pedicle screws and bone graft, which preserves muscle and shortens recovery.
My training encompasses both orthopedic and neurosurgical spine techniques, giving me deep expertise in nerve decompression and the ability to address complex cases that combine nerve compression with instability.
My Philosophy on Pinched Nerve Surgery
I'm conservative about surgery: I don't operate until conservative care has been genuinely exhausted, and when I do operate, I decompress thoroughly—removing all sources of compression—and fuse when the anatomy demands it. This approach maximizes relief, minimizes recurrence, and gets you back to your life without radiating pain or neurological deficit.
What to Expect From Decompression Surgery
Nerve decompression is typically performed under general anesthesia. I position you appropriately (prone for lumbar, supine or lateral for cervical), use real-time fluoroscopy to guide placement, and make small incisions over the affected segment.
For lumbar pinched nerves, I remove the lamina to open the spinal canal and enlarge the neural foramen. I remove bone spurs, thickened ligaments, and any disc material compressing the nerve root. I visualize the nerve decompression directly to ensure complete relief.
For cervical pinched nerves, I may approach from the front (anterior cervical discectomy if there's disc compression) or the back (posterior laminoforaminotomy if bone spurs are the primary problem). My approach depends on the exact anatomy of your compression.
If fusion is needed, I place pedicle screws and a rod (lumbar) or anterior plating (cervical) to stabilize the segment.
Most procedures take 1-2 hours per level. Many patients go home the same day or stay one night for observation.
Recovery after minimally invasive nerve decompression:
- Weeks 1-2: Rest, frequent short walks, pain management. Avoid bending and heavy lifting.
- Weeks 2-6: Gradual activity increase under brace support (if fusion). PT can begin.
- Weeks 6-12: Progressive strengthening, return to light activities. Most patients resume desk work around 4-6 weeks.
- Months 3-6: Return to normal activities, exercise, and full work duties. Nerve healing and sensory recovery may continue improving for several months.
Related Conditions
A pinched nerve often occurs alongside other spinal conditions. Learn more about herniated discs, sciatica, and specific surgical approaches like laminectomy-fusion and lumbar fusion.
Next Steps
If you're experiencing radiating arm or leg pain—particularly if it's accompanied by numbness, tingling, or weakness—don't assume you're stuck with it. A pinched nerve is highly treatable, whether through conservative care or surgical decompression.
My approach is individualized: we image your spine, examine you thoroughly, and build a treatment plan based on your specific anatomy, symptoms, and goals. Many patients improve dramatically with non-surgical care. Those who need surgery get the benefit of expert nerve decompression with minimal trauma and rapid recovery.
Schedule a consultation at my San Antonio or Houston office. We'll determine exactly what's compressing your nerve and chart the best path to relief.
Your radiating nerve pain doesn't have to be permanent. Let's fix it.
Common Symptoms
- Sharp or burning pain radiating along the compressed nerve pathway
- Numbness or tingling in the arm (cervical) or leg (lumbar) supplied by the affected nerve
- Weakness in the muscles controlled by the pinched nerve
- Pain that worsens with certain movements or positions
- Loss of sensation in the fingers, hand, toes, or foot
- Pins-and-needles sensation or electrical feeling along the nerve distribution
- Difficulty with fine motor tasks or gripping strength
- Pain that radiates from the neck or lower back to the limb
Treatment Options
- Physical therapy and core stabilization exercises
- Anti-inflammatory medications and muscle relaxers
- Epidural steroid injections to reduce nerve irritation
- Activity modification and postural correction
- Nerve decompression surgery (laminectomy or foraminotomy)
- Laminectomy-fusion for instability or recurrent compression
Frequently Asked Questions
What exactly is a pinched nerve?
A pinched nerve (radiculopathy) occurs when a nerve root is compressed as it exits the spine, usually by a herniated disc, bone spurs, or narrowing of the neural foramen. This compression causes radiating pain, numbness, or weakness along the nerve's path.
How long does it take for a pinched nerve to heal?
Most pinched nerves improve within 4-8 weeks of conservative treatment including physical therapy and anti-inflammatory care. Some cases resolve in weeks, while others may take 3-6 months. Severe cases may require surgery.
Can epidural injections help a pinched nerve?
Yes, epidural steroid injections are highly effective for pinched nerves. They deliver anti-inflammatory medication directly to the compressed nerve root, reducing swelling and pain. This relief window allows physical therapy to be more effective.
When is surgery needed for a pinched nerve?
Surgery is considered after 8-12 weeks of unsuccessful conservative treatment, or when neurological symptoms worsen. Progressive weakness or symptoms significantly limiting your daily activities warrant surgical evaluation.
What kind of surgery treats a pinched nerve?
Laminectomy or foraminotomy decompresses the nerve by removing bone or disc material compressing it. If instability is present, fusion stabilizes the segment. Dr. Cyr performs these procedures at his San Antonio and Houston offices with minimal-invasion techniques.

