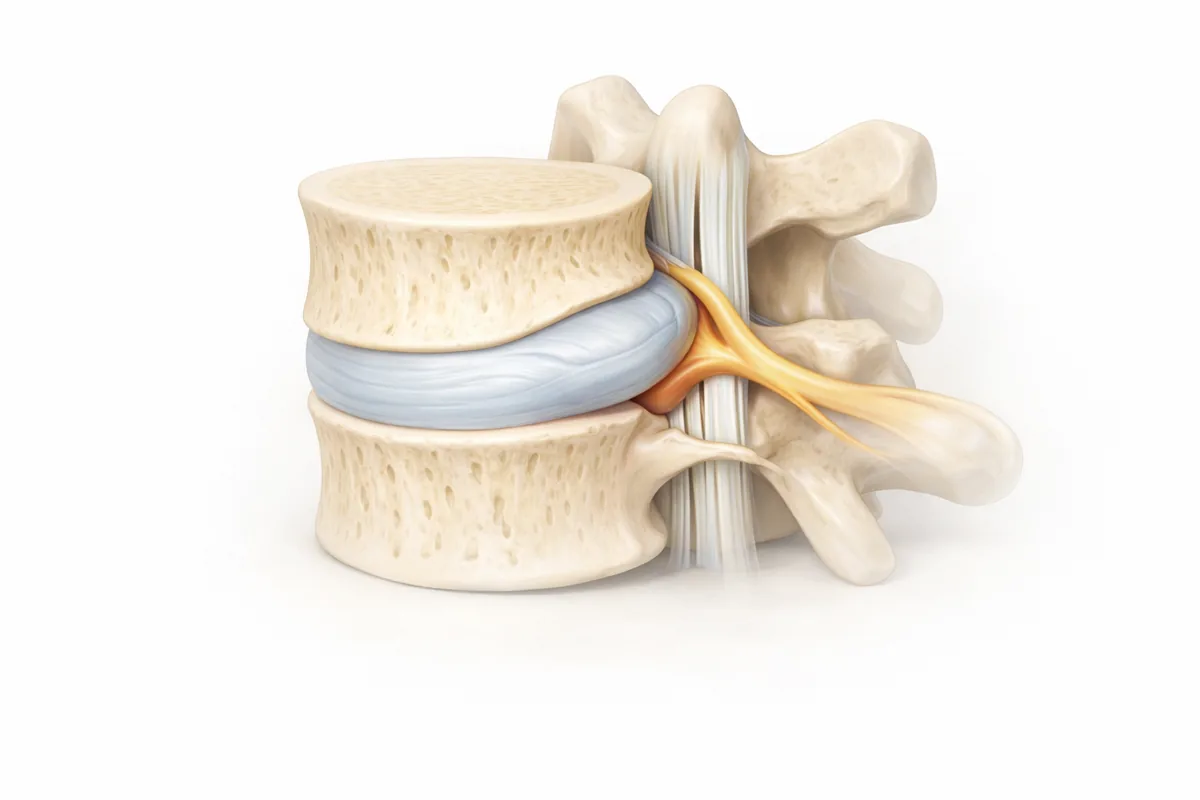
What Is a Bulging Disc?
Your spine is built like a stack of blocks—vertebrae separated by cushions called intervertebral discs. Each disc has a tough outer layer (annulus fibrosus) and a soft, gel-like center (nucleus pulposus). A bulging disc occurs when the entire disc extends uniformly beyond its normal boundary, pressing outward like a tire that's slightly overinflated.
This is different from a herniated disc, where the outer layer actually ruptures or tears, allowing the inner material to leak out in a localized spot. Think of it this way: a bulging disc is like the disc wall is thinning and pushing out evenly all around, while a herniated disc is like the wall has developed a hole.
Most bulging discs develop gradually over time due to aging, wear and tear, and the natural loss of disc hydration. While they're common—especially after 40—the good news is that many people with bulging discs never have pain or symptoms at all.
Why Your Disc Bulges
The spine works hard every day, bearing your body weight and absorbing the impact of movement, bending, lifting, and twisting. Over time, several factors can weaken the disc structure and cause bulging:
Degenerative Changes: As we age, intervertebral discs naturally lose water content and flexibility. The outer layer becomes less elastic, making it prone to gradual expansion.
Repetitive Stress: Jobs or activities that involve heavy lifting, frequent bending, or prolonged sitting create cumulative pressure on the discs over years or decades.
Poor Posture: Slouching or forward head posture shifts load unevenly onto the disc, accelerating wear.
Muscle Weakness: When your core muscles don't provide adequate support, your discs absorb more of your body's weight and movement stress.
Minor Injury or Trauma: Even small impacts or movements can accelerate disc changes in an aging spine.
Genetic Predisposition: Some people's discs simply age faster than others.
The key difference from a herniated disc is that in bulging, the disc material hasn't broken through the outer wall—it's just pushing against it. This is actually why bulging discs tend to respond so well to conservative treatment.
Bulging vs. Herniated: Why the Distinction Matters
Patients often use the terms interchangeably, but they're distinct conditions with different symptom patterns and treatment needs.
A bulging disc extends uniformly outward, like a tire bulging against a slightly-too-small wheel. The outer annulus is stressed but usually intact. Because the bulge is distributed around the disc's circumference, it may or may not irritate a nerve root. Many people have bulging discs on imaging but zero pain.
A herniated disc has a focal rupture—an actual breach in the outer layer that allows nucleus material to protrude into the spinal canal. This herniated material can directly compress nerve roots or the spinal cord, often triggering more acute, sharper pain and neurological symptoms like sudden numbness or weakness.
Why this matters for your treatment: Bulging discs typically respond beautifully to conservative care—physical therapy, activity modification, and time allow the disc and surrounding muscles to stabilize. The body often reabsorbs small amounts of herniated material, but the disc integrity is compromised, so treatment may take longer or be more cautious. Surgery is rarely needed for either condition, but when it is, a herniated disc with nerve compression is more likely to require intervention.
Common Symptoms of a Bulging Disc
Not everyone with a bulging disc feels pain. Imaging might reveal one during a scan done for an unrelated reason, and the patient never knew it was there. But when symptoms do occur, they typically include:
- Localized pain in the lower back, mid-back, or neck (depending on disc location)
- Pain worse with movement: Bending forward, twisting, or certain positions may aggravate the area
- Radiating pain, numbness, or tingling down the leg (sciatica-like) or down the arm, if the bulge presses on a nerve root
- Muscle stiffness or tightness around the affected area
- Pain that fluctuates: Some days worse than others, depending on activity and inflammation
In the cervical spine (neck), a bulging disc might cause neck pain, shoulder pain, or arm pain and numbness. In the lumbar spine (lower back), pain may radiate into the buttock and leg.
The severity of pain doesn't always correlate with the size of the bulge on imaging. A person with a large bulge might have no pain, while someone with a smaller bulge might be quite symptomatic. This depends on the exact anatomy of their spinal canal and how close the nerve roots sit to the bulging disc.
Conservative Treatment: Why It Works First
Here's why Dr. Cyr and most spine specialists start with conservative care for bulging discs: the condition often stabilizes on its own with the right support and modifications.
Physical Therapy
Targeted exercises strengthen the core muscles that support your spine and reduce the load on the disc. PT also improves flexibility and movement patterns, reducing stress on the bulging area. Many patients see significant improvement with 4-8 weeks of dedicated therapy.
Activity Modification
Avoiding positions and movements that aggravate your pain gives inflammation time to settle. This doesn't mean immobility—controlled, gentle movement is actually healing.
Anti-Inflammatory Medications
Over-the-counter NSAIDs (ibuprofen, naproxen) or prescribed medications reduce inflammation around the disc and nerve, easing pain and allowing healing.
Epidural Steroid Injections
When conservative care needs a boost, injecting corticosteroid around the inflamed nerve root reduces swelling and pain. This often works best within the first 6-12 weeks of symptoms and can buy time for the disc to stabilize.
Postural Training & Ergonomics
How you sit, stand, and move matters. Simple changes—better desk ergonomics, sleeping position adjustments, lifting technique—reduce disc stress significantly.
Heat and Rest
In acute phases, ice reduces inflammation. As pain subsides, heat supports muscle relaxation and blood flow.
When Surgery Becomes an Option
Surgery for a bulging disc is rare—less than 5% of cases need it. Dr. Cyr reserves surgical intervention for specific situations:
- Severe, unrelenting pain that hasn't improved after 6-12 weeks of aggressive conservative care
- Progressive neurological deficit: Growing weakness or numbness affecting function or strength
- Significant nerve compression confirmed on imaging with correlating symptoms
When surgery is needed, lumbar fusion or cervical fusion stabilizes the affected vertebrae and removes pressure from the nerve. Dr. Cyr's fusion approach prioritizes stability and long-term outcomes over temporary symptom relief.
What to Expect: Your Path Forward
Most patients with bulging discs recover well. The timeline depends on symptom severity, how long symptoms existed before treatment, and how diligently you engage in conservative care.
Typical recovery: 4-12 weeks for noticeable improvement; 3-6 months for substantial recovery. Some people continue gradual improvement for longer.
Key factors in your success:
- Consistent physical therapy participation
- Compliance with activity modifications
- Posture and ergonomic changes
- Stress management (stress tightens muscles)
- Patience—discs heal slowly
Next Steps
If you're experiencing back or neck pain and suspect a bulging disc, the first step is accurate diagnosis. Imaging (X-rays, MRI, CT) combined with a thorough physical exam confirms the problem. From there, a clear conservative care plan puts the odds in your favor.
Ready to explore your options? Dr. Steven Cyr specializes in spine conditions like bulging discs across San Antonio and Houston. He'll review your imaging, understand your goals, and build a treatment plan that starts conservatively but has a clear path to surgery if needed.
Learn more about herniated disc treatment to understand how that condition differs, explore our fusion procedure, or read when to see a herniated disc doctor.
Your spine is built to move and support you for life—with the right care, a bulging disc doesn't have to slow you down.
Common Symptoms
- Localized lower back or neck pain
- Pain that worsens with certain movements or prolonged sitting
- Radiating pain, numbness, or tingling down the arm or leg (if nerve compression)
- Muscle weakness or stiffness in the affected area
- Pain that may come and go
Treatment Options
- Physical therapy and targeted exercises
- Activity modification and postural training
- Anti-inflammatory medications
- Epidural steroid injections
- Heat/ice therapy and rest
- Spinal manipulation (when appropriate)
Frequently Asked Questions
Is a bulging disc the same as a herniated disc?
No. A bulging disc extends uniformly outward without rupture, while a herniated disc has a tear allowing inner material to protrude. Bulging discs typically cause more localized pain and respond better to conservative treatment.
Do I need surgery for a bulging disc?
Surgery is rare for bulging discs—less than 5% require it. Most respond well to physical therapy, activity modification, and anti-inflammatory treatment. Surgery is only considered for severe, unrelenting pain or progressive neurological loss.
How can I manage bulging disc pain at home?
Rest during flare-ups, apply ice acutely or heat for chronic pain, take NSAIDs to reduce inflammation, avoid aggravating movements, and maintain gentle mobility. Physical therapy should begin as soon as pain permits.
What's the recovery timeline for a bulging disc?
Most patients see noticeable improvement in 4-12 weeks with consistent conservative care. Full recovery typically takes 3-6 months. The disc gradually stabilizes as supporting muscles strengthen through physical therapy.
Can a bulging disc get worse?
Yes, without proper treatment a bulging disc can progress to herniation or cause increasing nerve compression. That's why early physical therapy and activity modification are important to prevent progression.

