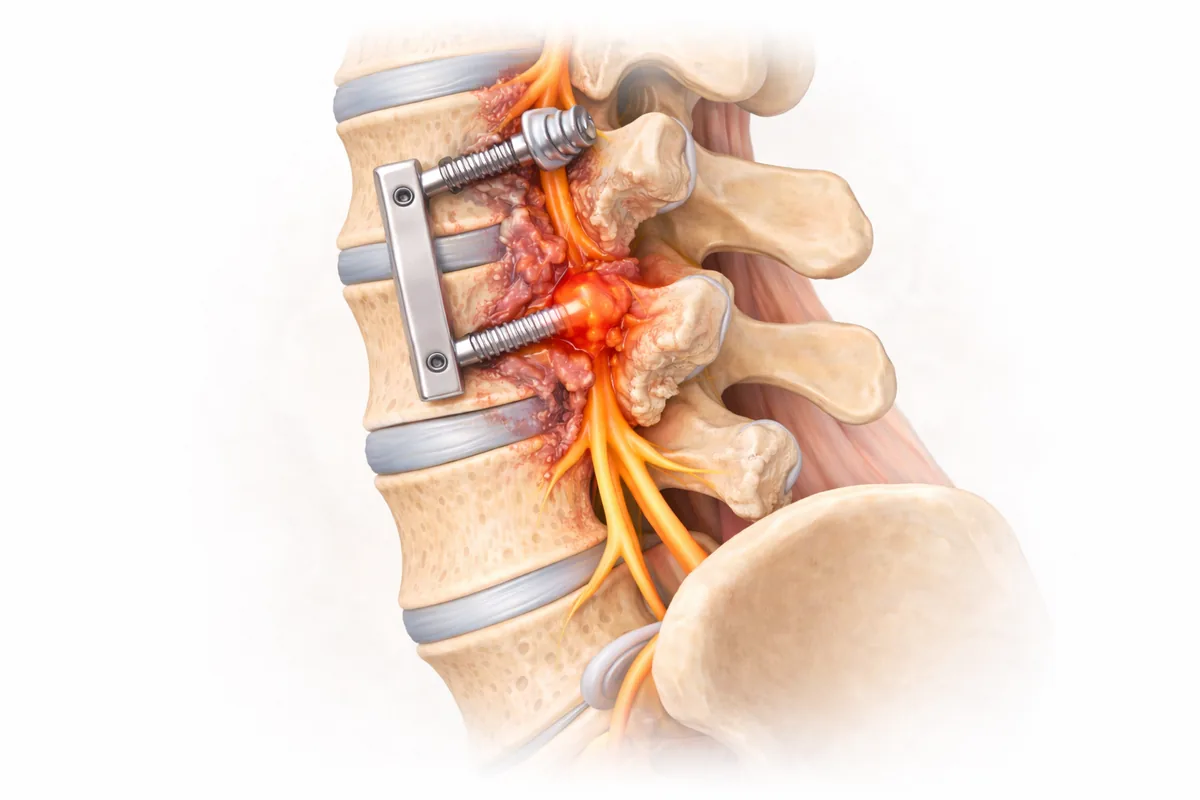
You had spine surgery to fix your back pain. You waited through recovery, did your physical therapy, and believed the pain would finally go away. Instead, months or even years later, you're still hurting—or the pain has returned in ways you didn't expect. You're not alone, and it's not your fault.
Failed Back Surgery Syndrome (FBSS) is a real condition that affects 10-40% of spine surgery patients. The good news: there are answers, and there are options. Dr. Steven Cyr specializes in exactly this situation—helping patients like you understand what went wrong and find a path forward.
What Is Failed Back Surgery Syndrome?
Failed Back Surgery Syndrome refers to persistent or recurrent pain after spine surgery, even when the surgery was technically successful on paper. It's often misunderstood: it doesn't mean the surgeon made an obvious mistake. Instead, it means the pain problem is more complex than the first surgery addressed.
This can happen for several reasons. Sometimes the surgery treated the wrong level of the spine. Other times, inadequate decompression—not removing enough bone or disc material—left the nerve under pressure. In some cases, the body's natural healing response creates scar tissue (epidural fibrosis) that irritates nerves. Adjacent segment disease can develop above or below the surgery site. Hardware can fail. A disc can re-herniate. And occasionally, the original pain source was never the real problem—there was another issue that wasn't recognized.
The frustration FBSS patients experience is real. You did what you were told to do. You trusted the process. And yet, here you are, still in pain and now wondering if any surgery can truly help.
How Do You Know You Have Failed Back Surgery Syndrome?
FBSS symptoms vary depending on which nerves are involved and what's causing the problem:
Pain patterns often feel different from your pre-surgery pain. Some patients describe a burning sensation, others a sharp stabbing pain. The location may shift—pain that was in your lower back now radiates into your leg. Some patients feel fairly good most days, then have flare-ups that disable them.
Neurological symptoms—numbness, tingling, weakness in your legs or feet—suggest nerve involvement. You might notice your leg gives out when you walk, or you have difficulty with stairs.
Functional limitations persist despite surgery. Walking, sitting, or standing may remain painful or limited. The relief you expected never materialized.
The key difference: these symptoms appear weeks, months, or years after surgery, often after you'd already started to improve or felt the surgery was helping.
Getting an Accurate Diagnosis
This is where many FBSS patients get stuck. A general physician or even a non-specialist spine surgeon may not have the expertise to dig into what's really causing your ongoing pain. They might tell you to live with it, that "surgery isn't the answer," or recommend another surgery without fully investigating the problem.
Dr. Cyr takes a different approach. As a Mayo Clinic-trained orthopedic spine surgeon with extensive revision surgery experience, he knows that FBSS requires careful detective work.
The process begins with your surgical history. Dr. Cyr thoroughly reviews your operative reports, imaging from before your first surgery, and post-operative imaging. What exactly was done? At which level? What was the stated goal? Understanding the intent behind the first surgery is crucial.
Advanced imaging is essential. An MRI with contrast, or a CT scan with contrast, can reveal scar tissue, nerve compression, disc recurrence, or problems with hardware. These images tell a story that plain X-rays might miss.
Diagnostic injections can pinpoint where your pain originates. A targeted injection near a suspected problem area can briefly relieve your pain, confirming that location as the pain source. This is invaluable for planning treatment.
Your Treatment Options
Not every FBSS patient needs surgery. Many respond well to conservative care, especially when the underlying cause is accurately identified.
Physical therapy and activity modification can be surprisingly effective if nerve compression or instability is mild. A skilled therapist familiar with post-surgical spines can help strengthen supporting muscles and improve movement patterns.
Pain management techniques—epidural steroid injections, facet joint injections, or medial branch blocks—can provide relief and reduce inflammation around irritated nerves. These are often part of a broader pain management plan.
Spinal cord stimulation (neuromodulation) is an increasingly popular option for patients whose pain doesn't respond to conservative care. A small device sends electrical pulses to interrupt pain signals before they reach your brain. It's reversible, adjustable, and can be life-changing for the right candidate.
Revision spine surgery becomes the right choice when imaging and diagnostic injections identify a structural problem—a recurrent disc herniation, inadequate decompression, instability, or another issue—that conservative care won't fix. At that point, fixing the problem is often more effective than living with pain management alone. For cases involving lumbar instability, a lumbar fusion approach may be the appropriate solution.
Why Choose Dr. Cyr for Your FBSS?
Dr. Cyr's expertise in revision and complex spine surgery isn't incidental to his practice—it's central to who he is as a surgeon. He understands the anatomy of the previously operated spine, the challenges of navigating scar tissue, and the importance of precise diagnosis before recommending surgery.
More than that: he understands the emotional weight of FBSS. He knows his patients are often frustrated, afraid of another "failed" surgery, and exhausted from chronic pain. He listens carefully, explains options clearly, and never pushes surgery as the only answer. His goal is to help you understand your situation and find the right solution for you.
Whether you're in San Antonio or Houston, Dr. Cyr is available for a comprehensive second opinion consultation. He'll review your records, perform a detailed examination, answer your questions, and outline what he believes is the best path forward—whether that includes surgery or not.
The Path Forward
Failed Back Surgery Syndrome is not a death sentence. It's not a reason to resign yourself to permanent pain. It's a sign that your spine problem was more complex than initially recognized, and it requires a more sophisticated approach to diagnosis and treatment.
You deserve an expert who takes the time to understand your unique situation. Dr. Cyr has spent his career helping patients in exactly your position reclaim their lives.
Ready for a second opinion? Schedule a consultation with Dr. Cyr at our San Antonio or Houston office. Bring your surgical records and recent imaging. Let's figure out what's really going on and what your options are.
Your story doesn't have to end here.
Common Symptoms
- Persistent or recurrent pain months or years after spine surgery
- New pain patterns different from your original problem
- Numbness, tingling, or weakness in legs or feet
- Pain that radiates down the leg (sciatica-like symptoms)
- Muscle weakness or difficulty walking
- Stiffness or reduced mobility despite surgery
Treatment Options
- Comprehensive surgical record review and second opinion
- Advanced imaging (MRI, CT scans with contrast)
- Diagnostic injections to identify pain source
- Physical therapy and conservative management
- Spinal cord stimulation and neuromodulation
- Revision surgery when structural problems are identified
Frequently Asked Questions
Why do I still have pain after my spine surgery?
Failed Back Surgery Syndrome affects 10-40% of spine surgery patients. Pain can result from inadequate decompression, scar tissue, the wrong level being treated, or an unrecognized problem. The underlying cause varies and requires careful diagnosis.
Is revision spine surgery safe?
Yes. Revision surgery is more complex due to scar tissue, but when the underlying problem is accurately identified and addressed, outcomes are good. Dr. Cyr specializes in revision surgery with extensive experience navigating previously operated spines.
Do I need another surgery or can conservative care help?
Not all FBSS requires surgery. Many patients improve with physical therapy, injections, or spinal cord stimulation. Dr. Cyr's thorough diagnostic process identifies which patients benefit from conservative care versus surgical revision.
What is spinal cord stimulation?
Spinal cord stimulation (neuromodulation) uses a small device to send electrical pulses interrupting pain signals. It's reversible and adjustable. It's an excellent option for patients whose pain doesn't respond to conservative care and who wish to avoid revision surgery.
Can I get a second opinion from a revision surgeon in Houston?
Yes. Dr. Cyr offers specialized second opinion consultations for FBSS at his Houston office (9125 West Road). Bring your surgical records and imaging. He'll review what was done and outline your options—whether surgical or non-surgical.

