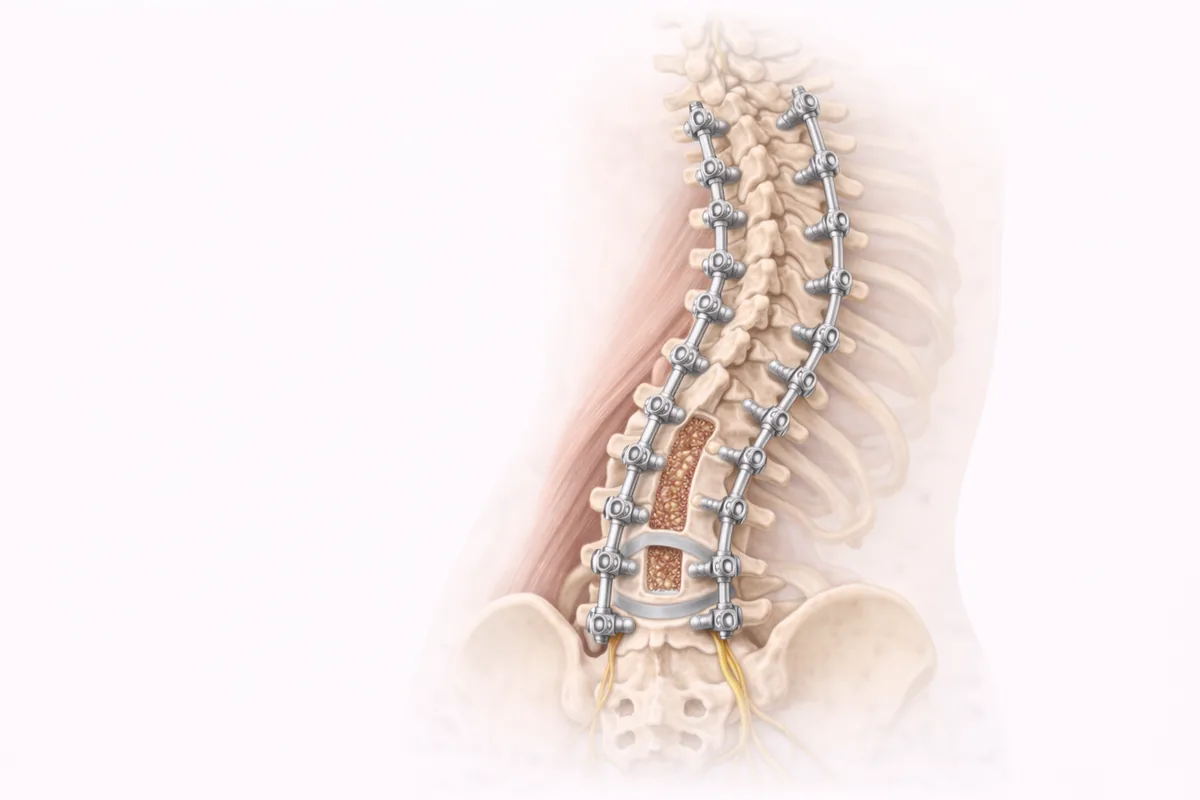
About Scoliosis Surgery
Scoliosis—an abnormal sideways curvature of the spine, which may manifest as levoscoliosis (leftward curve) or dextroscoliosis (rightward curve)—can progress silently for years. When a curve becomes severe or begins causing pain, neurological compromise, or cardiopulmonary effects, surgical correction offers the only definitive treatment.
I've dedicated a significant portion of my spine surgery practice to scoliosis correction because it remains one of the most rewarding procedures I perform. Straightening a severely curved spine requires meticulous planning, sophisticated instrumentation, and surgical technique refined over decades. The payoff—watching patients stand taller, move freely, and return to activities they thought were lost—never gets old.
My background includes specialized fellowship training at Mayo Clinic in both orthopedic and neurological spine surgery, along with my service as Chief of Spine Surgery for the United States Air Force. That dual expertise shapes how I approach scoliosis: I think like an orthopaedic surgeon about alignment and biomechanics, and like a neurosurgeon about nerve protection and neurological recovery.
Who Benefits from Surgery
Not every curve requires surgery. Mild curves (less than 25–30 degrees) in skeletally immature patients are typically managed with observation and sometimes bracing. Surgery is recommended when:
- Curves exceed 45–50 degrees and risk of further progression is high
- Adult degenerative scoliosis causes pain, weakness, or walking imbalance
- The curve compresses lung capacity or affects heart function
- Neurological symptoms (numbness, weakness, loss of fine motor control) develop
- Quality of life is significantly impaired despite conservative care
Adolescent idiopathic scoliosis, adult degenerative scoliosis, and neuromuscular scoliosis each require different surgical strategies—a distinction I assess carefully at the initial consultation.
My Approach to Scoliosis Correction
Every scoliosis spine is unique. Before surgery, I obtain detailed imaging (X-rays, CT, sometimes MRI) and assess spinal flexibility using supine and side-bending films. This tells me how much correction is realistic and which fusion levels will optimize long-term outcomes.
I believe in maximizing curve correction while minimizing fusion length. Fusing fewer levels preserves spinal motion, reduces stress on adjacent discs, and allows for more natural movement after recovery. When appropriate, I use minimally invasive approaches to reduce soft-tissue trauma and accelerate healing.
My Mayo Clinic training emphasized avoiding over-correction—we don't straighten spines artificially; we correct them to physiologic alignment. This reduces the risk of long-term complications and improves patient satisfaction with cosmetic and functional results.
What Happens During Surgery
Scoliosis correction typically involves a posterior spinal fusion with pedicle screw instrumentation. I make a midline incision over the affected spinal segments, expose the vertebrae, and use specialized instruments to realign the spine. Then I secure the correction using titanium screws and rods, followed by fusion of the vertebral bodies using bone graft.
For severe curves or specific patient factors, I may recommend an anterior-posterior approach (fusing from both front and back) or an anterolateral technique. Each method has advantages depending on curve location, magnitude, and underlying pathology.
The procedure typically takes 4–6 hours, depending on complexity. Neurophysiologic monitoring throughout surgery helps ensure no nerve damage occurs. Many patients stay 2–3 nights in the hospital, though some well-selected candidates go home sooner.
Recovery Timeline
- Weeks 1–2: Pain management and gentle movement; avoid bending and twisting.
- Weeks 3–6: Progressive physical therapy; return to light activities (walking, stationary cycling).
- Weeks 6–12: Continued strengthening; most patients resume desk work and driving.
- 3–6 months: Majority of restrictions lifted; return to sport and heavy activity as tolerated.
- 1 year: Maximum benefit of surgery realized; fusion solid on imaging.
I provide detailed post-operative protocols and close follow-up. Most patients report significant pain relief and improved function by 3 months post-surgery.
I treat patients from across Texas and beyond who travel to San Antonio or Houston for their procedure. My goal is straightforward: restore your spine's alignment, eliminate pain, and help you reclaim your active life.
Learn more about scoliosis | Levoscoliosis | Dextroscoliosis
When This Procedure Is Recommended
- Abnormal spinal curvature visible from behind
- Uneven shoulders, hips, or ribcage
- Back pain that worsens over time
- Shortness of breath or heart palpitations
- Leg pain or neurological symptoms from curve progression
Surgical Techniques
- Posterior Spinal Fusion with Instrumentation
- Anterior and Anterolateral Fusion Techniques
- Minimally Invasive Correction
- Revision Scoliosis Surgery
- Selective Fusion (preserving spinal motion segments)
Frequently Asked Questions
How long will the scoliosis correction last after surgery?
Once fused, the corrected spine segments will not move again. Unfused segments above and below the fusion continue normal motion. Maintaining good posture and core strength helps ensure long-term stability.
Will I lose flexibility after scoliosis surgery?
Yes, fused segments won't move—that's the point. However, the remaining mobile spine often compensates well. Most patients feel more flexible after surgery once pain improves and they begin physical therapy.
What are the risks of scoliosis correction surgery?
Serious complications (infection, major nerve injury, pseudarthrosis) occur in less than 5% of cases in experienced hands. Minor complications (transient pain, superficial infection, temporary nerve irritation) are managed routinely. All risks are discussed at consultation.
Can I have more surgery later if needed for scoliosis?
Yes. Revision scoliosis surgery is possible, though it's more complex. Good surgical technique the first time minimizes the need for revision.
What if my scoliosis curve comes back after surgery?
True recurrence of a solid fusion is rare. However, degenerative changes can develop above or below the fusion over decades—a phenomenon called adjacent-segment disease. This is rare and often asymptomatic.

